Third and Fourth Degree Tears during Childbirth
What are the types of tears during childbirth?
Approximately 90% of women tear to some extent during childbirth. Most tears occur in the perineum, the area between the vaginal opening and the anus (back passage). They may be:
- First degree tears – small skin-deep tears which usually heal naturally
- Second degree tears – deeper tears affecting the muscles of the perineum as well as the skin. These usually require stitches.
For some ladies with a tear, the tear may be more extensive. This may be:
- A third degree tear, extending downwards from the vaginal wall and perineum to the anal sphincter, the muscle that controls the anus.
- A fourth degree tear, extending to the anal canal as well as the rectum (further into the anus).
This information is for you if you have had a third or fourth degree tear and aims to answer some frequently asked questions about how to manage your stitches and have a good recovery.
What is the difference between an episiotomy and a tear?
According to the Royal College of Obstetricians and Gynaecologists, an episiotomy is a cut made by a doctor or midwife through the vaginal wall and perineum to make more space to deliver the baby. A tear happens as the baby stretches the vagina during birth.
What is the treatment for a third and fourth degree tear?
A third or fourth degree tear is repaired in an operating theatre, either with a general or regional anaesthetic such as a spinal or epidural. This allows the doctor to ensure that the muscles are well drawn back together and to ensure adequate pain relief.
What are the short and long-term effects of a third or fourth degree tear?
Most women make a good recovery. 60-80% of women will be free of symptoms 12 months after delivery. However, during recovery, some women may experience:
- Loss of control of the bowels/wind
- Pain or soreness in the perineum
- Fears and apprehension about having sex – lubrication may help with this
- A feeling of needing to rush to the toilet to open their bowels urgently
- Fear about a future pregnancy and birth.
It is important to speak to a health care professional such as a midwife, consultant or pelvic health physiotherapist if you have any concerns so that they can advise you accordingly.
How can I look after the wound?
It is important that you keep the area as clean as possible. Have a shower or a bath at least once a day. Long soaks in the bath should be avoided as they can cause the stitches to dissolve too early. Scented bubble baths and shower gels may irritate this area and are best avoided. Pat dry rather than wipe.
Maternity pads are softer and thicker than normal sanitary pads and may be more comfortable. These should be changed at regular intervals (washing your hands both before and after you do so).
Stitches usually dissolve and fall out by the time the cut or tear has healed but occasionally they have to be taken out.
Pain management
Ice therapy may be beneficial in relieving pain. Place a few ice cubes or a pack of peas in a plastic bag and wrap them in a damp towel (do not place ice directly on the skin as this will burn). Place the ice pack over the stitches for a maximum of 10-15 minutes. This can be repeated as many times a day as needed.
Painkillers can help. However, if you are breastfeeding, check with your pharmacist, midwife or GP before you buy over-the-counter painkillers.
Contact your midwife or general practitioner if:
- Your stitches become more painful or smell offensive. This may be a sign of infection
- You cannot control your bowels or wind
- You feel the need to rush to the toilet to open your bowels
- You have any other worries or concerns.
Pelvic floor muscle exercises
These muscles are positioned at the base of the pelvis. They support your internal organs and are also important in controlling your bladder and bowel. Doing regular pelvic floor muscle exercises will aid the healing process by increasing blood flow to the area. It is not uncommon for women to find that control of the bowel and bladder is affected after a third or fourth degree tear. It is important to exercise these muscles regularly to prevent unwanted leakage of urine when you cough, sneeze or exercise (‘stress incontinence’) or wind or faeces from the bowel. It is beneficial and safe to do pelvic floor muscle exercises after your catheter has been removed.
To exercise the pelvic floor:
For endurance:
- Sit comfortably on a chair with both feet flat on the floor
- Imagine you are trying to stop yourself passing wind and the flow of urine at the same time. It feels like a ‘squeeze and lift’
- Do not tighten your buttocks or hold your breath when doing this exercise
- Try and hold the lift for up to four seconds
- Relax for four seconds.
You will also need to practice short and strong contraction:
- Squeeze and lift the pelvic floor as strongly as you can, then relax. Repeat this four times.
Remember to tighten these muscles before a cough or sneeze, or before lifting.
Pelvic floor exercises may be uncomfortable to start with, but never painful. If you experience pain, then make sure that you focus on relaxing the muscles fully and try again the next day.
As your tissues heal and get stronger, gradually begin to increase the length of time that you hold until eventually you can hold for the count of eight. Also gradually increase the number of repetitions until you can do eight long and strong (endurance exercises) and eight short and strong exercises.
Do not practice these exercises when emptying your bladder (stopping mid-flow). This can be used as a very occasional test, but never first thing in the morning.
To ensure the best possible results, and reduce the risk of incontinence problems in the future, pelvic floor exercises should be practised three times a day and ideally every day for the rest of your life.
Advice for opening your bowels
After third and fourth degree tears, it is particularly important to avoid constipation and to ensure that you have formed, but soft, bowel movements (stools). Type 3-4 (see chart below) is the recommended consistency of stool. If your stools are too loose (Type 5-6),
they may be difficult to control. If your stools are too hard (Type 1-2), they can be painful and difficult to pass and could potentially cause further damage.
You will be provided with laxatives to help your stools to be soft and easy to pass. It is recommended that you have a varied and healthy diet with plenty of fluid and fibre, including fruit and vegetables. It is important to drink at least 1.5 to 2 litres of fluid evenly spread throughout the day (six to eight mugs).
You can read the Bristol Stool Chart below.

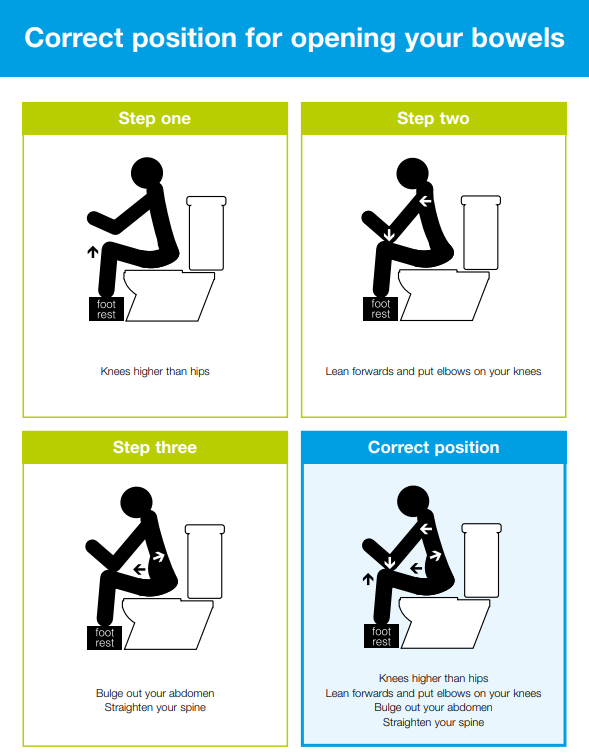
The following diagram demonstrates the correct position for opening your bowels. It shows the use of a footstool so that your knees are slightly higher than your hips. You may also find it helpful and more comfortable to apply a gentle, upwards pressure externally over the perineum (between the vagina and the back passage), using a pad of toilet paper to support the stitches.
Sexual activity
There is no right or wrong time to resume sexual activity after pregnancy and/or childbirth after a third/fourth degree tear. It is important that both you and your partner feel relaxed and ready. If there are no problems then sexual activity can be resumed when stitches are healed and bleeding has stopped. Some women prefer to wait until their six week postnatal check.
It is not unusual for sex to feel different and a little uncomfortable initially, but this should not last. A water soluble lubricant may help to begin with, especially if you are breastfeeding or your vagina feels drier than normal. If you experience persistent pain or discomfort, ask your GP or physiotherapist for advice.
What happens after I leave hospital?
You will be given an appointment in a Gynaecology Clinic approximately 12 weeks after delivery. At this appointment the consultant will discuss any problems or concerns you may have. This appointment is very important as it will help with the plan of care for the delivery of your future babies and ensure your continuing good health. It is a good idea to write down any questions that you may have to bring to this appointment.
It is also routine practice to have a physiotherapy appointment at approximately six to eight weeks after delivery. You will be sent a letter asking you to contact the Physiotherapy Department to book an appointment. The physiotherapist will check whether you are doing your pelvic floor exercises correctly and help you to strengthen your muscles if needed.
They will also give you advice if the healing scar is still tender.
It is very important for you to attend both of these appointments even if you are well and have no symptoms.
Contact numbers
We hope that you have found this information useful. If you have any questions or are worried about anything, please speak to the following Dorset County Hospital staff:
Jane Lofts or Christina Leadley: 01305 255314
Physiotherapy Department: 01305 255314
Useful websites
Maternity Matters: https://maternitymattersdorset.nhs.uk/
Royal College of Gynaecology: https://www.rcog.org.uk/for-the-public/browse-our-patient-information/care-of-a-third-or-fourth-degree-tear-that-occurred-during-childbirth-also-known-as-obstetric-anal-sphincter-injury-oasi/
About this leaflet
Authors: Jane Lofts, Highly Specialised Uro-Gynae Physiotherapist and Christina Leadley, Pelvic and Obstetric Health Physiotherapist (reproduced with kind permission of Norgine group of companies)
Written: September 2019
Approved: March 2020
Review date: March 2023
Edition: v1
If you have feedback regarding the accuracy of the information contained in this leaflet, or if you would like a list of references used to develop this leaflet, please email patientinformation@dchft.nhs.uk
Print leaflet