Having a Gastroscopy with an Oesophageal Stent
What is a gastroscopy?
A gastroscopy is a look at your gullet, (called ‘oesophagus’), stomach and first part of your bowel (called ‘duodenum’).
The instrument used to do the examination is called a Gastroscope. It is a flexible tube with a bright light and a tiny camera at the tip that transmits pictures of the inside of your oesophagus, stomach and duodenum to a video screen. It is inserted through your mouth.
Why have a gastroscopy?
The purpose of a gastroscopy is to see if there are any abnormalities of the oesophagus, stomach or duodenum. The video pictures will show any areas of inflammation or other abnormality.
The Gastroscope has a hollow tube inside that can be used to take samples of tissue (called biopsies). These can be looked at in the laboratory under a microscope.
What is an oesophageal stent?
An oesophageal stent is a specially designed metal mesh-like tube. It is designed to be placed in the oesophagus (gullet) across a narrowed area. When it is being positioned, it is thin (about the size of a pencil). When the doctor has positioned it in the right place, it then expands to press against the gullet to make the narrowed area wider. Once the stent is in place, it usually remains there permanently, although some stents can be removed if necessary.
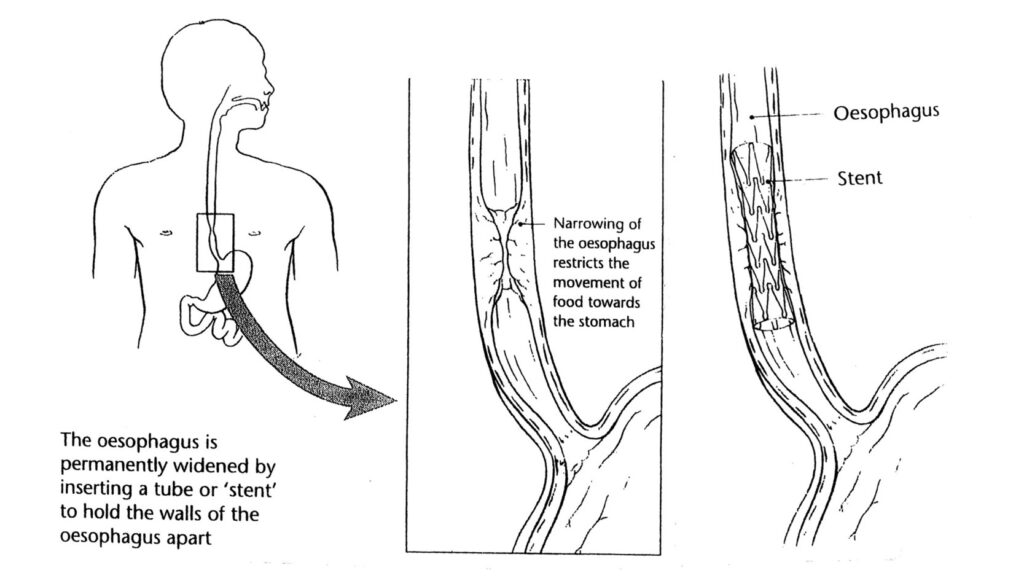
Why should I have a stent?
A stent is recommended to people who have a narrowed area in their oesophagus (gullet) who have difficulty swallowing. This can be distressing for you and those around you. Often you may have had increasing difficulty in getting food down. This often gets more difficult until swallowing fluids becomes a problem. This is when a stent may help.
The purpose of the stent is to widen your oesophagus enough to enable you to eat soft food and drink again.
The narrowing is often caused by cancer. If you are at all unsure what is causing your narrowing, please ask to speak to your doctor or specialist nurse.
Is there an alternative?
Having a stent put in is your choice, and it is important that you are happy with the decision to have one. Whatever you decide, your decision will be respected.
Eating and drinking are an essential part of living. The aim of the stent is to allow you to swallow again. If you decide against this, and nutrition can no longer be swallowed the normal way, there are currently other alternatives to a stent, although these are not appropriate for everyone.
Alternatives are radiotherapy or chemotherapy. Your consultant will be able to discuss these alternatives with you in detail. Some people choose not to have any treatment.
What are the risks?
As with any procedure, there are risks involved, and it is important that you are aware of them to enable you to make the right decisions about your treatment. The risks will vary depending on exactly where the narrowing is and the type of stent used.
It is common to feel slightly ‘windy’ immediately following the procedure but this settles very quickly.
Risk of inhaling stomach contents – This is why we ask you not to eat or drink for six hours before your appointment (during the procedure any moisture in the mouth can be removed using a small suction tube: like at the dentist.
Risks from Sedation – Sedation medication can affect the breathing but in order to minimise any risk your dose is individually assessed and your oxygen level monitored throughout the procedure.
If you are asthmatic or have any breathing difficulties, please inform the nurse on your arrival and bring your inhalers with you.
It is rare, but an allergic reaction to medications can occur and will need medical treatment.
Risk of damage to teeth or bridgework – Please advise the nurses before the procedure if you have any broken or loose teeth, dentures are removed before the procedure.
Risk of sore throat – You may experience an unusual sensation in your throat for a day or two afterwards.
Risk of Bleeding – There is a small risk of bleeding occurring when the stent is put in, this can happen in around 1 – 2 in 100 people but is not usually a major problem. A trace of bleeding noticed in saliva or a black stool is not unusual and should not cause alarm.
Risk of perforation – If this happens; it may cause an infection and require a repositioning of the stent and insertion of a drain.
Another risk is of the stent slipping out of place. This can happen in 2 – 3% of people but if it happens the stent can usually be safely re-positioned.
Discharge advice will be discussed with following your procedure.
If any of these complications occur, your doctors will explain exactly what is happening, you would be monitored closely and may need to remain in hospital a little longer than planned.
Preparing for your oesophageal stent
The stent is put in place in the Endoscopy Unit and takes about 15 – 20 minutes.
Do not have anything to eat or drink six hours before your appointment.
Planning your care
If you are taking any of the following medications or have the medical conditions listed here, please contact the Clinical Advice Line on 01305 253152 to help us plan appropriate care and management of your condition during your visit with us:
| Do the following apply? | If yes: |
| Do you have a long-term condition such as epilepsy, Parkinson’s, chronic pain and steroid deficiency e.g., Addison’s (adrenal deficiency)? | Call Clinical Advice Line |
| Diabetes | Call appointments to ensure an appropriate appointment; see diabetic leaflet |
| Recent heart attack Cardiac pacemaker or ICD fitted Are you pregnant? | Call Clinical Advice Line |
| Aspirin or Dipyridamole therapy | Continue as normal |
| Warfarin therapy | You will receive written instructions on when to stop these medications |
| Clopidogrel, Ticagrelor, Prasugrel therapy | |
| Dabigatran, Rivaroxaban, Apixaban, Edoxaban therapy | |
| Anti-hypertensives to lower your blood pressure | Call Clinical Advice Line |
| Diuretics (water tablets) | |
| NSAID’s (non-steroidal anti-inflammatory drugs), such as Ibuprofen or Meloxicam |
What happens when you get to the Endoscopy Unit
When you come to the Endoscopy Unit please give your name to the receptionist.
A nurse will take you through to a private office. You will be asked some questions about the arrangements you have made to get home and about your health. The nurse will check your breathing, pulse and blood pressure, if you take Warfarin your INR will be checked, and if you are diabetic your blood sugars will be checked. Please tell the nurse if you are allergic to any medicines.
You can ask any questions that you have or tell the nurse of any worries. It is not unusual to feel anxious about having an oesophageal stent inserted. The nurses and endoscopists understand this and will do their best to reassure you.
Once the nurse has finished taking your details you will be asked to sit back in the waiting area. When the endoscopist is ready to see you, a nurse will come and take you through to get changed into a hospital gown.
Signing the consent form
You will have been sent a consent form as part of your admissions pack, please read this before your procedure. You will have a chance to speak to your endoscopist before the procedure to discuss any concerns, and to sign the consent form. Please bring this form with you on the day.
The endoscopist or a senior endoscopy nurse will meet and talk to you about the procedure. It is important before signing that you understand what is likely to happen. You will be given time to ask any questions that you may feel necessary to make up your mind.
What are the key things to remember?
It’s your decision and you can choose whether or not to consent to what’s being proposed. Ask as many questions as you like and remember to tell the team about anything that concerns you or about any medication, allergies or past medical history which might affect your general health.
How the stent is put in
There are many people involved in providing safe stent insertion. After you enter the room the nurses will go through a final checklist with you. You will be asked to lie on your back on a trolley so that a small needle can be placed in your hand or arm to allow us to give you medication for the procedure. Most stenting procedures are conducted using heavy sedation given by an anaesthetist. Alternatively, you may be given a combination of a sedative to make you sleepy, a painkiller to keep you comfortable, and a muscle relaxant to help control the movement of the gut. These do not make you unconscious, although many patients are very sleepy within a few minutes. You may have some awareness during the procedure however most people do not remember anything and are comfortable throughout.
You will be asked to remove any false teeth, spectacles or contact lenses. Your pulse, blood pressure, breathing rate, oxygen levels and heart rhythm will be monitored throughout the procedure. To do this we will place a soft clip on your finger, a cuff around your upper arm, and stickers on your back. We will also give you oxygen via a mask. You will then be asked to turn over onto your front. A mouth guard will be placed between your teeth and gums to protect them and to prevent damage to the endoscope.
The stent is carefully positioned. When the consultant is happy that it is in exactly the right place they will allow it to expand.
Immediately after the stent has been inserted you will stay in the Endoscopy Unit Recovery Area.
When you have recovered sufficiently you will be taken on a trolley to a ward.
The stent begins to expand straight away but will continue to expand for up to 48 hours. During this time, you may experience some discomfort or pain. The degree of this varies from person to person and is not possible to predict. If you do feel pain, it is important that you tell the nurses so that they can give you painkillers.
After 48 hours, the discomfort or pain usually lessens. Many people do not need to take any more painkillers, but some people continue to experience a pain that needs longer-term pain killing medicine. Whilst in hospital, your doctors can see what pain relief you have needed, so that when you go home, you will be given a further supply.
The stent is keeping the oesophagus open and at times this can allow acid from the stomach to splash back into the oesophagus, which can cause pain. You will be prescribed medication to reduce the amount of acid in the stomach to overcome this.
Your GP will be sent a letter telling them that you have had a stent put in and what medicines you were sent home with, so that they can prescribe further supplies for you.
How long will I have to stay in hospital?
Everyone is different, but most people have the stent put in and then go home 24 – 48 hours later. Occasionally it is necessary to stay a few days longer. Before going home, your doctors will want to make sure that you are comfortable and that you are managing to eat.
Patients’ property
You are advised not to bring expensive items of jewellery or clothing with you when you visit the Endoscopy Unit.
You will be given a patient property bag to place your clothes in if you need to change for your procedure.
You will be asked to keep your property with you at all times.
The Endoscopy Unit and Dorset County Hospital NHS Foundation Trust cannot accept responsibility for the safeguarding of your property.
Please note: individuals are unable to donate blood for four to six months after flexible endoscopy and until they have informed the blood service of the diagnosis.
What should I eat?
After the stent has been put in place, it is very important that you learn how to look after your stent by eating the right things.
The dietician will see you to make sure you know what you should be eating, and that you are having an adequate diet.
The dietician may also recommend nutritional supplements if necessary and advice on how to get further supplies. It is important that you eat an appropriate diet to avoid the stent becoming blocked.
Diet information
Foods that are to be avoided:
- Stringy /hard raw vegetables
- Fruit skins, stringy pith of citrus fruit
- Tough meat and gristle
- New or crusty bread
- Fish with bones
- Nuts and dried fruit
- Hard chips
- Any food that becomes a lump in your mouth.
Suggested meal plan
Breakfast
- Porridge, Ready Brek, Weetabix, Rice Krispies with milk and sugar
- Soft fruit, e.g. banana, stewed apple, ripe pear or melon
- Thick and creamy yogurt
- Glass of fruit juice.
Main meal
- Tender meat or meat substitute in gravy eg shepherds pie, corned beef hash, chicken stew
- Fish in sauce, e.g., parsley or butter, Fishermans pie
- Tender meat or vegetable curry with rice.
- Mashed potato with added butter, cream or cheese
- Soft well cooked vegetables, e.g. carrots, cauliflower, swede.
Snack meal
- Jacket potato (no skin) with butter and soft filling, e.g. tuna or salmon with mayonnaise, tinned spaghetti, grated cheese, cream cheese
- Soup with added cream, cheese, skimmed milk powder or tender meat.
Desserts
- Milk pudding e.g., rice pudding
- Sponge pudding and custard, cream or ice cream
- Thick and creamy yogurt
- Trifle, Angel delight, mousse.
Between meal snacks
- Milky drinks e.g., milky coffee, hot chocolate, Horlicks.
- Biscuits
- Plain soft cake e.g. sponge cake
- Suggested desserts (as above).
Additional comments
Because some people can swallow more easily than others, the dietary advice will also vary from one person to another.
The following foods may be safe for people who can still swallow quite easily:
- Toasted brown bread (small portions without the crusts) – brown is less sticky than white
- Runny egg yolk and soft poached eggs (scrambled egg and cooked egg whites can be too ‘rubbery’ and may block the stent)
- Melba toast and bread sticks (small portions and well-crunched up)
- Crisps that dissolve and melt in the mouth e.g. Cheese Puffs, Skips, Quavers.
The above is for information only. It is best to follow your dietician’s instructions. If you have any queries, please ask your dietician for further advice.
If you don’t feel hungry
If you have a poor appetite or have lost some weight try the following:
- Eat little and often, including small snacks
- Choose full cream milk and full fat foods instead of low fat products
- Add sugar to cereals, puddings and drinks
- Grated cheese, cream or butter can be added to mashed potatoes, soups, sauces and puddings
- Fortify milk by adding 2 – 4 tablespoons of dried milk powder to 1 pint of milk. Use this for drinks, soups, puddings and sauces
- Try a nourishing drink suck as Complan, build up or supermarket own brand or make your own fruit smoothie or milkshake.
- There are nutritional products which can be prescribed by your doctor if you continue to lose weight. These are available in a variety of flavours and consistencies. Your dietician can offer more information and advice.
What else you can do to avoid problems after having a stent
The two most important things are:
- Take small mouthfuls and chew for longer than usual
- Make sure your teeth are in good order. If you have dentures make sure they fit correctly. Visit the dentist if necessary so that you can chew more effectively. If you find it difficult to chew, have foods that are already soft.
Other things that will help are:
- Crush any tablets or better still ask your doctor or pharmacist for liquid medicines
- Drink during and after meals, to clear the stent of any food particles. Warm fluids may help the most, but any fluid is beneficial
- Sit up straight when eating. This allows gravity to help food go down. Sit upright for half an hour after meals
- Cut food into small bits before eating. It is important that you don’t swallow hard lumps of food that could block the stent
- Have plenty of gravy, custard or cream with your food to make it moister and help it go down more easily
- Try to relax when eating and do not rush your meals; it may help to eat smaller amounts more often
- Don’t be afraid to spit out lumps that can’t be chewed
- Mix any powdered supplements thoroughly, as lumps of powder can block the stent.
What to do if you think the stent is blocked
- It’s important that you stay calm
- Stop eating – don’t try and force it down
- Try to drink small amounts – warm water or fizzy drinks can be helpful and walk around
- If it does not clear after three hours, contact your GP, specialist nurse, or go to your local Emergency Department
- Stop trying to drink anything at this time
- If the blockage does not go, you may need to be admitted to hospital. If this happens, it is likely that you will have a drip put in your arm to give you fluids so that you don’t become dehydrated whilst not able to swallow fluids. If the blockage doesn’t go, you will then probably need to have a gastroscopy to see if your stent is blocked.
Useful organisations
These are some useful organisations with their telephone numbers and websites that you may wish to contact.
Macmillan is a charity that provides information and support for patients and their families. They also produce booklets that are free to patients at https://www.macmillan.org.uk/
Useful booklets are:
- Understanding cancer of the Oesophagus.
- Diet and the cancer patient.
- Coping with fatigue.
To talk to someone or request a book telephone 0808 808 0000.
Oesophageal Patients Association is a national charity formed by former oesophageal cancer patients to share experiences, give advice and support. They are able to offer over the telephone support and advice and also produce useful written advice.
Website: https://www.opa.org.uk/
Telephone: 0121 704 9860
e-mail: enquiries@opa.org.uk
NHS
https://www.myhealth.london.nhs.uk/your-health/cancer/my-cancer-treatment
https://www.nhs.uk/pages/home.aspx
The Endoscopy Unit and Dorset County Hospital NHS Foundation Trust cannot accept responsibility for the content of any information obtained from the internet.
Contact numbers
Endoscopy Unit main reception: 01305 255225
Appointment enquiries: 01305 255701
Clinical Advice Line (medical enquiries): 01305 253152
If you call the Clinical Advice Line and your call goes to answer phone, please leave a message with the following details:
- Your name and telephone number
- The procedure you are having
- Date and time of your appointment
- Your reference number (hospital number) or our reference number (NHS number)
- Your query.
Someone will return your call as soon as possible to discuss your telephone message with you.
If you are using hospital transport and your appointment is after 2pm, please contact the appointments line to rearrange an earlier appointment.
About this leaflet
Author: Caroline Angel, Endoscopy Charge Nurse, Dinsdale Marjoram
Written: January 2026
Approved: January 2026
Review date: January 2029
Edition: v2.1
If you have feedback regarding the accuracy of the information contained in this leaflet, or if you would like a list of references used to develop this leaflet, please email patientinformation.leaflets@dchft.nhs.uk
Print leaflet