Having a Gastroscopy Feeding Tube (PEG Feeding)
What is a Gastroscopy Feeding Tube?
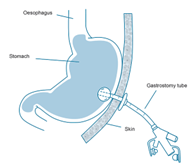
A gastrostomy tube is a feeding tube designed for people who require tube feeding over a longer period of time. It is a small plastic tube which is inserted directly into the stomach, through the skin and can be discreetly hidden under the clothes. It allows you to receive liquid feed, water and sometimes medication directly into the stomach, without having to swallow.
Is it my decision to have a tube feed?
Yes. The decision is yours. The doctors, dietitians and your relatives will discuss it with you and help you to decide along with the GP, speech and language therapist, community nurse and specialist nurse (if applicable).
What are the benefits to me?
Tube feeding can provide you with good nutrition, which can improve your sense of wellbeing and help your body fight infection.
Tube feeding can reduce any anxiety related to being unable to eat well throughout the day. Although tube feeding does not give the same pleasure as eating, it can relieve feelings of hunger or thirst, and may make you feel less tired.
Tube feeding can also help reduce the risk of chest infections, which can occur when food or drink accidentally passes into the airways or lungs during swallowing.
How is the tube inserted?
The tube is inserted during a minor operation at the hospital and is usually under a local anaesthetic and light sedative (medication that makes you drowsy).
For the tube insertion you may attend the Endoscopy Unit, or X-ray Department or occasionally the Operating Theatre.
If you attend the Endoscopy Department for the tube insertion you will have a tube called a PEG inserted. The term PEG is used to describe the way the tube is inserted. PEG stands for:
PERCUTANEOUS (through the skin)
ENDOSCOPIC (instrument used to examine the stomach)
GASTROSTOMY (opening into the stomach)
- The PEG tube is approximately ¼ inch (1/2cm) thick and 12inches (30cm) long. Rather like a piece of spaghetti made of soft plastic with a hole down the middle. Ask your dietitian if you would like to see a tube.
- The procedure is performed by a specialist doctor in the hospital using a dastroscope (a flexible instrument used to examine the inside of the stomach).
- The whole process takes about 30 minutes to complete.
- As this is a minor surgical procedure you may have some discomfort for a few days afterwards. You will be given medication to help this.
- If you have any questions about the procedure, ask your doctor/nurse or dietitian.
What are the risks of the procedure?
Having a tube inserted does carry a risk of complications. As with any treatment the risks must be weighed against the benefits. To minimise these risks, you will be assessed for suitability before the procedure by your doctor or hospital specialist, and these will be discussed with you.
The most common complication is wound infection. As with any invasive procedure there is a risk of infection (10%, 1 person in 10). Antibiotic cover is given prior to the procedure.
While inserting the feeding tube there is a small (1%, 1 person in 100) risk of internal bleeding which usually settles on its own. Also, there is a small risk of puncturing the bowel. If this happens it may mean the Gastrostomy tube will have to be removed. Rarely, an operation to repair the bowel will be needed.
After PEG insertion there is a small (less than 1%, 1 person in 100) risk of leakage from the tube into the abdomen. This can lead to a condition called Peritonitis.
There are risks related to the sedation which can affect your breathing. However, using a light sedative can minimise these risks. You will be monitored closely during and after the procedure.
Some abdominal pain may be experienced after the procedure, but this should settle, and you will be given pain relief.
In a small number of cases (up to 5%, 1 person in 20). Endoscopic assessment will show that it is unsafe to insert a PEG Tube. In this situation, the procedure will be stopped and at a later stage your doctor will discuss an alternative surgical or radiological technique of safely inserting a feeding tube into the stomach.
If you have any concerns, please discuss them with your doctor.
Planning your care
If you are taking any of the following medications or have any the medical conditions listed here, please contact the Clinical Advice Line on 01305 253152 to help us plan appropriate care and management of your condition during your visit with us:
| Do the following apply? | If yes: |
| Do you have a long-term condition such as epilepsy, Parkinson’s, chronic pain and steroid deficiency e.g., Addison’s (adrenal deficiency)? | Call Clinical Advice Line |
| Diabetes | Call appointments to ensure appropriate appointment; see diabetic leaflet |
| Recent heart attack Cardiac pacemaker or ICD fitted Are you pregnant? | Call Clinical Advice Line |
| Aspirin or Dipyridamole therapy | Continue as normal |
| Warfarin therapy | You will receive written instructions on when to stop these medications |
| Clopidogrel, Ticagrelor, Prasugrel therapy | |
| Dabigatran, Rivaroxaban, Apixaban, Edoxaban therapy | |
| Anti-hypertensives to lower your blood pressure | Call Clinical Advice Line |
| Diuretics (water tablets) | |
| NSAID’s (non-steroidal anti-inflammatory drugs), such as Ibuprofen or Meloxicam |
How soon after the tube insertion can I start feeding?
The Endoscopy Unit will send instructions back with you to the ward. It normally states feed can commence after six hours. The feed is introduced slowly to begin with, so that your body can adjust to the feed.
How will I be fed by tube?
There are two main ways:
- By BOLUS FEEDING – the liquid feed is drawn up in a 50ml syringe and then slowly syringed into the PEG tube at various intervals during the day. This can be time consuming and therefore not suitable for everyone.
- Via A PUMP – this is the standard way of feeding in hospital and at home. The tube on the outside of your stomach has a special adaptor which fits onto the feeding set (called a giving set). The feeding set is connected when you need to be fed and disconnected at other times.
The feeding set is made up of the following:
- The feed which is usually in 500, 1000 or 1500ml containers.
- A plastic tube with a connection on one end for the feed container and the other for the adaptor on your gastrostomy tube.
- The pump, which is used to regulate the rate of feed being dripped into your stomach.
The pump can be worked by battery or from the mains electricity supply.
What feed will I receive?
You will receive a prescribed, commercially prepared liquid feed which contains all the essential nutrients you will need daily. Your dietitian will recommend the type and amount of feed that you will need.
You may receive part or all your daily food via you gastrostomy tube, depending on your specific medical condition and needs.
Liquidised food should never be put down the tube as this is likely to block it.
Who supplies the feeds?
Before discharge from hospital the dietitian will contact your GP, requesting that they prescribe the feed for you. The GP will then write out a monthly prescription for the feed. The dietitian can arrange for the feed and equipment required to be delivered by a Home Care Company to your home, or it can be delivered to a local pharmacy.
The Home Care Company will supply the giving sets and either the Home Care Company or your district nurse will supply the syringes. This depends on your local health authority.
The hospital dietitian will explain which system you will be using.
How much do the feeds cost?
The feed is only available on prescription; therefore, you pay the normal prescription cost (unless you are exempt from paying for prescriptions).
Will I be able to take anything by mouth?
Just because you have had a gastrostomy tube (PEG) fitted it does not necessarily mean that you have to stop eating and drinking. This will depend on your condition and treatment. If you have swallowing difficulties, your speech and language therapist will advise you whether it is safe for you to eat and drink and what types of food and drinks are suitable.
If I am not eating anymore, do I still have to look after my mouth?
Your mouth must be looked after even if you are not eating. Plaque can build up very quickly, so it is essential to brush your teeth at least twice daily. A saline mouthwash is usually recommended for good mouth health.
Pineapple juice-soaked gauze squares can be used for cleaning the mouth – the enzyme in the pineapple is effective in removing plaque.
How will I take my medication?
If you are finding it hard swallowing your medication it can be taken via the gastrostomy tube (PEG), rather than orally. The medication will be prescribed in liquid form and administered down the PEG tube using a syringe.
The tube should be flushed with water before and after each medication (approximately 50mls) to prevent the tube blocking. NEVER crush tablets and syringe them down the tube.
Having the feeding tube can often make it easier to make sure you receive all your medication.
Who looks after the tube?
It is important to consider this before the tube is placed. Giving feed and medication through the tube and care of the tube require daily attention. Some individuals manage the tube and feed themselves, while others need support from relatives, carers and healthcare professionals.
The time spent attached to the feeding set will depend on the amount of food you need and your lifestyle. You will be able to discuss this and the best pattern for you with your dietitian.
There are portable feeding sets for those who need feeding away from home.
How long will I need the tube for?
This really depends on the individual, but the tubes can last for more than five years if looked after properly. A replacement tube can be inserted often without the need for a further operation.
How will I care for the tube?
The tube should be flushed with at least 50mls of freshly run tap water before and after the feed or medicine administration, to prevent blockage of the tube. Your dietitian will advise on the type of water to be used.
You should only use the tube to administer the prescribed feed, water and liquid medication.
Will I be able to take a bath or shower?
You will need to wait until the site (called the ‘stoma’) is fully healed before you can bathe or shower as normal (this may take a few weeks).
Meanwhile, the site should be cleaned with cooled, boiled water and dried, then left without a dressing covering the site (if covered this can encourage infection).
The gastrostomy tube (PEG) and attachments can be cleaned with water.
Sometimes the Stoma oozes and may need cleaning more than the normal twice a day. When you clean your teeth, clean the stoma (have a routine).
After that period, it is perfectly acceptable to have a bath and shower. Check the tube and attachments for wear and tear and make sure the tube is closed and the clamp applied when not in use.
Can I go swimming?
Yes. It is advisable to cover the site with a waterproof dressing when swimming in public pools. Make sure the end is closed and the clamp applied. The district nurse will be able to advice you on the appropriate dressings.
What about sexual relationships?
Having a gastrostomy tube (PEG) should not interrupt your home life, and this includes personal and sexual relationships. You can still share your bed with your partner, and it shouldn’t interfere with sex or get damaged. It may help to secure it with your dressing tape to prevent it getting pulled.
Will the gastrostomy tube (PEG) be in forever – is it reversible?
You may not need a gastrostomy forever. If it is no longer being used or necessary then, yes, it can be reversed or removed. Your hospital team, community dietitian, district nurse or GP can help arrange this. You would need to return to the Endoscopy Unit at your local hospital, where it is quickly removed.
Can a PEG fall out?
The PEG is fixed by an internal disc within the stomach so it cannot easily fall out. It can be secured with a dressing tape or within the clothes to prevent it getting pulled.
What happens if the tube falls out or gets pulled out?
You should either phone your GP, the Endoscopy Unit or go to the nearest Accident and Emergency Department as soon as possible to get another tube put in. If you leave it too long the incision could start to close.
What problems might I encounter?
Tube problems:
- Blockage
- Inflammation of the skin
- Infection
- Leaking
- Displacement
Feed Problems:
- Diarrhoea
- Constipation
- Nausea
- Vomiting.
You will be trained on how you can avoid these problems. Your dietitian will advise you on how to deal with feeding issues if they arise.
What do I do if I have problems?
You will be given training and written information on how to care for the tube and contact numbers of people to phone if you run into problems. You will be given this before you leave hospital.
How will it affect my life?
As with anything new, a tube feed may change your routine and may mean you have to consider different things. It may take time to adjust to these changes.
If being fed via a pump, you will be connected to the pump for a set period of time and, therefore, many people choose for this to be done overnight. This way it does not interrupt daily activities. However, some people prefer to be fed during the day.
Talk to your dietitian on how best to include tube feeding into your existing lifestyle. It can be tailored to your individual needs.
On discharge from hospital, you will not be left to cope alone. There are many health professionals within your local community available to support you. It does depend on you and/or your carer’s ability to manage the tube feeding. If you or your carers are intending to be responsible for the gastrostomy tube, initially the district nurse will visit to offer help and assistance until you are fully confident. If, however, you are not in a position to look after the PEG then it is often possible for the district nurse to come into your home, to help you.
The dietitian will monitor your tolerance to the feed and weight etc. and will provide follow up appointments with them and the speech and language therapist (SALT), if applicable. This can take place at the PEG Clinic at the hospital where you will also see a nurse who will check your gastrostomy tube and stoma site for any problems.
If you are unable to attend the clinic, then home visits can be arranged. The feed and Homecare Company also have a helpline. Your GP will also offer support and provide you with your monthly feed prescription.
Making the decision
Having read this leaflet and considered the need for a tube feed, you now need to consider if tube feeding is in your best interests.
Sometimes this can be a very difficult decision to make, you may feel you need to discuss it in further detail. Your care team will be happy to talk through any issues you, your relatives or carers may have.
We are privileged to be a training hospital
There may be a trainee endoscopist observing or performing your procedure. If this is the case, there will also be a fully trained accredited Endoscopist present. You will be informed during your admission. You do have the right to decline their participation in your procedure; please let the admitting nurse know of your wishes.
Your appointment time is the time you are expected to arrive in the department. However, you should plan to be in the Endoscopy Unit for three to four hours, unless you have been notified that you will stay overnight. The department has three procedure rooms running at the same time also accommodates emergencies. Someone with a later appointment time may be seen before you. If you have any concerns, please ask a member of staff.
Contact numbers
Endoscopy Unit main reception: 01305 255225
Appointment enquiries: 01305 255701
Clinical Advice Line (medical enquiries): 01305 253152
If you call the Clinical Advice Line and your call goes to answer phone, please leave a message with the following details:
- Your name and telephone number
- The procedure you are having
- Date and time of your appointment
- Your reference number (hospital number) or our reference number (NHS number)
- Your query.
Someone will return your call as soon as possible to discuss your telephone message with you.
If you are using hospital transport and your appointment is after 2pm, please contact the appointments line to rearrange an earlier appointment.
About this leaflet:
Author: Dinsdale Marjoram
Written: January 2026
Approved: January 2026
Review date: January 2029
Edition: v2
