Breast Lymphoedema
This leaflet explains what swelling (lymphoedema) of the breast is, why breast lymphoedema develops, how it is recognised, and information on how it can be managed.
It is common to develop some swelling in the breast after surgery and/or radiotherapy, but this usually settles and reduces after a few weeks. Sometimes the breast swelling may persist after the initial six to eight weeks and can develop with or without arm swelling.
There may also be changes to your breast as a result of your treatment, such as shape and size changes, scarring and differences between your breasts.
There are several risk factors which may increase your risk of developing breast lymphoedema:
- The number of lymph nodes removed from the armpit (axilla)
- Radiotherapy to the breast/axilla
- Post-surgical complications such as infection, seroma (collection of fluid), and cording (tightness or pulling of cords in the axilla)
- Lack of support to the breasts
- Large or pendulous breasts (cup size larger than C)
- Being overweight.
Signs and symptoms
You may notice that your breast feels heavier or hard (fibrosed) in places. There may be altered sensation, changes in skin colour, fullness, or discomfort. You may notice marks left on your skin from bra straps or seams.
Managing breast lymphoedema
Breast lymphoedema can be successfully managed using a number of different approaches. Learning how to self-manage is the most successful approach to treatment.
- Skin care – it is important to look after your skin to reduce the risk of infection (cellulitis). Wash and dry the breasts thoroughly, this is especially important between and under the breasts, and in any skin folds. Using a non-perfumed moisturiser can help to keep the skin intact and hydrated.
- Bra fitting – it is important to wear a bra that fits you well and provides a full cup with firm support. The bra should be non-wired. This will help to lift and support the breast and reduce the build up of fluid. Sometimes it can be helpful to wear a sleep/soft cup bra overnight to support the breast and prevent further fluid build-up. This is particularly important for large breasts.
- Exercise – keeping active and exercising is important to help the muscles pump lymph fluid more effectively through your body and therefore reduce swelling. Movement helps you improve and maintain flexibility and keeps your bones strong. It can help you maintain or achieve a healthy weight and may improve your emotional well-being. Try to use your arm and shoulder normally and continue your arm exercises as advised prior to your surgery/radiotherapy. It is important to maintain good posture. Deep breathing exercises will also be beneficial.
- Weight management – try to keep your weight within normal limits. If you are overweight, try to reduce your weight as this will improve lymphoedema.
- Lymphatic massage – Simple lymphatic drainage (SLD) is a form of self-massage using specific techniques to move and redirect fluid from the swollen area to unaffected areas. Your lymphoedema Nurse will advise you if this is indicated. The website link for a YouTube video is: www.lymphoedema.org/information/self-management-videos/ Select SLD for breast/chest wall lymphoedema.
- Medical tape – this is an adhesive tape which may be applied to encourage drainage in the swollen breast. Your lymphoedema nurse will discuss this with you if indicated.
- Foam/padding – this can be worn inside the bra to add more support and compression to the breast.
Tips to ensure you are wearing the correct bra
A well-fitting supportive bra is essential to support the breast and allow fluid to drain. It is important to be remeasured after your treatment to ensure you are wearing the correct size and aim to return to a supportive bra as soon as any discomfort settles down after treatment. It is advisable to be re-measured annually as any change in weight will alter your bra size.
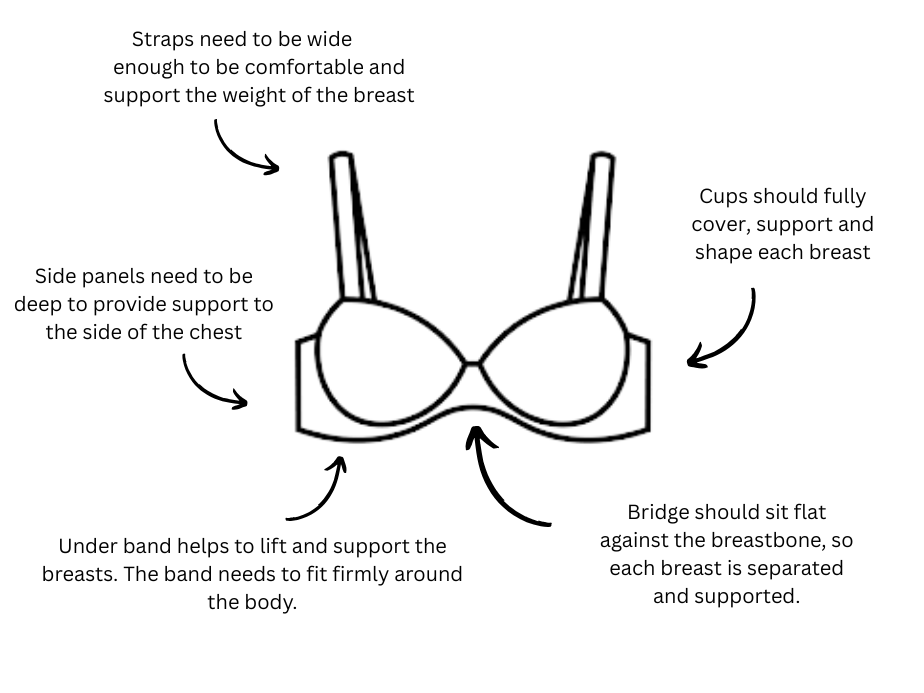
Make sure the band of your bra fits firmly but comfortably around the narrowest part of your back. The band provides the main support. You should just be able to fit two fingers under the band once it is fastened. It should not ride up at the back. The band and the side support should sit flat against the body and around the contour under the breast. The side section should be wide/deep enough to provide maximum support to this area.
Both breasts should fit neatly into the cups. Nothing should be spilling out below or over the top (cup too small). There should be no wrinkling of the fabric (cup too big). The middle part of the bra should sit flat against your body.
Before you adjust the straps check that the breasts are in a natural position (usually half way between the shoulders and elbow). The straps should not dig in or slip off the shoulder. Choose a bra with wide straps and regularly check and adjust the straps as washing and wearing can loosen straps. If wearing a prosthesis, it is important to ensure that your bra is supporting your natural breast.
Types of bras that may be suitable
Firm non-wired support bras with deep cups, wide supportive straps, and wide under band side panels. Sports bras with moulded supportive non-wired cups that apply good compression over the breasts.
Putting your bra on properly
The best way is to put the straps on first, then lean forward and place your breast inside the cups. Next fasten the hook on your back and adjust the cups and your breast tissue slightly so that your breasts are comfortable and well supported.
Contact numbers
We hope that you have found this information useful. If you have any questions or are worried about anything, please speak to the Lymphoedema Specialist Nurses:
Emma Diaz 01305 255370
Dawn Johnston 01305 255370
Lucy Harris 01305 255370
Useful websites
Breast Cancer Now – www.breastcancernow.org
Lymphoedema Support Network – www.lymphoedema.org/
Cancer Research UK – www.cancerresearchuk.org/about-cancer/breast-cancer/living-with/lymphoedema-after-treatment
About this leaflet
Author(s): Dawn Johnston
Written: September 2025
Approved: November 2025
Review date: November 2028
Edition: v1
If you have feedback regarding the accuracy of the information contained in this leaflet, or if you would like a list of references used to develop this leaflet, please email patientinformation.leaflets@dchft.nhs.uk
Print leaflet