Minimally Invasive Glaucoma Surgery (MIGS) Devices (iStent inject and Hydrus microstent)
This leaflet will help you understand a bit more about the newer micro-surgical options for glaucoma. The two MIGS devices / implants that we currently offer at the Eye Department at Dorset County Hospital NHS Trust are the iStent inject implant and the Hydrus microstent.
This leaflet explains what the operation involves, the benefits and risks, and what you should do afterwards. This information is designed to help you decide whether you would like to have this surgery. It will also make you aware of what to expect when you come to the hospital.
If you would like additional information about the what the surgery involves, please speak to one of the doctors or nurses. They will be more than happy to help.
What is glaucoma?
Glaucoma is an eye condition that can affect sight, usually due to a build-up of pressure within the eye. This eye pressure is known as intraocular pressure (IOP). If it is not treated or if treatment is delayed, it can cause blindness.
A fluid (called aqueous humour) is produced inside the eye. This fluid is needed to provide nutrients to the front of the eye, especially the cornea and lens. It also removes waste products from the eye.
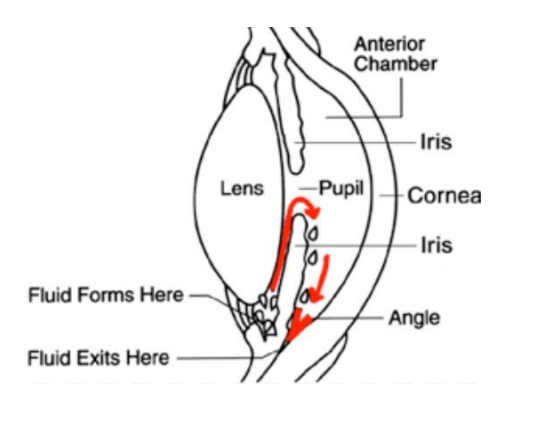
The fluid drains mainly through a structure called the trabecular meshwork. This meshwork lies in the angle where the cornea meets the iris. Please refer to the image on the left. The red arrows show how the fluid (aqueous humour) circulates in the eye
The normal pressure in the eye is between 10 and 21 millimetres of mercury (mmHg). If, for any reason, the fluid is blocked and cannot get out, the pressure can rise, and glaucoma may occur
What treatment options and alternatives are there?
There are various treatment options including eye drops, laser treatment and drainage surgery. Surgeries include the minimally invasive glaucoma surgeries also known as MIGS. MIGS include iStent implant and Hydrus implant. Other surgeries for glaucoma are more complex, some of these are trabeculectomy, Preserflo microshunt and Glaucoma drainage device (GDD or tube shunt) implantation.
Your consultant will discuss relevant options with you, and you can decide which option you prefer. You do not have to have treatment – it is your decision. However, if glaucoma is not well controlled, it may cause blindness.
Please note that almost all glaucoma treatments and procedures, including laser treatments, are to control your eye pressures and glaucoma. These are not aimed to improve your vision. Once vision is lost from glaucoma, you cannot get it back. All treatment for glaucoma is aimed at slowing down the rate of progression of glaucoma, to reduce the risk of blindness during your lifetime.
Let us now learn more about the iStent inject implant and the Hydrus microstent implant, collectively referred to here as MIGS implants
What is iStent?
The iStent is a small (about 0.36 mm long) titanium tube that is implanted into the eye to lower intraocular pressure and reduce the need for eye drops in patients with glaucoma. It is currently the smallest device implanted in the human body.
What is Hydrus?
A Hydrus microstent is a tiny (about 8mm long), tube-shaped implant that is implanted into the eye to lower intraocular pressure and reduce the need for eye drops in patients with glaucoma. It is roughly the size of an eyelash. It is made of nitinol, which is flexible and biocompatible.
How do iStent and Hydrus work?
Glaucoma is usually caused by raised pressure within the eye. This occurs due to reduced drainage of fluid (aqueous humour) through the eye’s natural drainage channels.
The MIGS implants are inserted into the eye’s natural drainage channel – the trabecular meshwork. The aqueous humour is then able to drain through these devices. Insertion of these MIGS implants involves a short surgical procedure that is often done at the same time as cataract surgery. It can also be done as a stand-alone procedure. It is usually performed under local anaesthesia as a day case procedure.

Why have the iStent or Hydrus implant?
The aim of the MIGS procedures is to reduce intraocular pressure and reduce the need for glaucoma eye drops.
These implants will not cure your glaucoma. They will not reverse any damage to your vision that has already occurred. The goal is to reduce the risk of blindness from glaucoma in your lifetime.
MIGS implants are not suitable for all types of glaucoma. They may not be suitable for all stages of the disease. and are not suitable for all stages of the disease. It is most suited for people with mild to moderate open angle glaucoma. Your consultant will have a chat with you about whether and which implant may be suited to your case.
Other benefits of MIGS implants
The surgery is less invasive compared to other more complex drainage surgeries. It also has a faster recovery time.
It provides an extra option for controlling glaucoma where glaucoma medications, laser treatments or other complex glaucoma surgeries are not appropriate.
The MIGS implants are made from biocompatible materials, so they will not be rejected by your body. They do not cause an allergic reaction.
They will not set off airport scanners and in most circumstances, they will not cause any problems if you need to have an MRI scan.
What are the risks of MIGS implants?
Although they have been approved for use, these are relatively new procedures. There is still a lot to learn about them. Some of the safety issues may not be known. We are continually examining the outcomes for patients who have these implants, so that we can understand more about it.
A very small amount of bleeding inside the eye occurs during the operation but this clears up within a few days. There is a risk of the eye becoming inflamed and developing an infection, so you will be given anti-inflammatory and antibiotic eye drops to use after the operation to prevent this.
In some cases, the implants may not lower the eye pressure. However, if this happens it will not create any additional harm to your eye. The procedure is regarded as safe. The risk of sight threatening complications is less than the more invasive glaucoma procedures and considered similar to that of cataract surgery.
Are there any alternatives?
Alternatives include other glaucoma surgeries, but they carry more risk than these minimally invasive procedures. Your doctor will be able to discuss this further
Preparing for the operation
You should continue using any eye drops and tablets for your glaucoma as prescribed until your operation. Your doctor will discuss this with you. If you take any blood-thinning medicines (e.g. warfarin) please discuss this with the doctor or nurse.
Before the operation you may be asked to attend a pre-operative assessment appointment. This is check that you are fit for the procedure and anaesthetic. You may have a blood test taken and other tests done to check your general health. Please bring an up-to-date list of your medications with you to this appointment. If you are unsure of anything, please check with your GP.
During the operation
The operation is usually performed with a local anaesthetic, which means that you will be awake. However, we will numb your eye so you will not feel anything.
The procedure usually takes less than 60 minutes if done along with cataract surgery. It is often performed at the end of cataract surgery but can also be done separately. The standalone procedure usually takes less than 30 minutes. The device is implanted through a tiny incision made in the eye. It is inserted into the eye’s natural drainage channel with a special injector.
After the operation
After the operation, your eye will be covered by a protective plastic shield. You can remove the shield the next morning and gently clean your eye.
At the time of discharge, you will be given different eye drops to use for four weeks. These help the eye to recover from the operation. We will usually provide you with sufficient drops and these should last at least
Going home
The iStent and Hydrus implant procedures are performed as day case procedures which means that you will go home on the same day.
It is very important that you do not bump, rub or press your eye after surgery. You should also avoid swimming for four weeks until your wound has healed.
The length of time you will need off work depends upon the nature of your job. Most people need one to two weeks off after surgery. If your job involves heavy manual work or you work in a particularly dusty/dirty environment you may require longer. Please discuss this with your doctor/nurse.
A self-certifying sick note is required for the first seven days of absence. This is available from your employer or GP, not from the hospital. After this period, a medical sick note is required; this is available from your GP or hospital doctor.
There are no long-term restrictions following MIGS surgery, so once your wound has healed and you feel normal, you may be able to carry on your activities as normal.
Follow up
You will be reviewed in the eye clinic one week after your operation and then again at week three and week six. It is very important that you attend all your clinic appointments and use your eye drops as prescribed.
Symptoms to report
Contact us immediately on one of the numbers below if:
- You have any loss of vision
- Your operated eye becomes increasingly red or painful.
Contact numbers
Eye casualty triage: 01305 254837
Ophthalmic secretary via Dorset County Hospital switchboard: 01305-255103
Please attend the Emergency Department or call 111 if out of hours or during weekends.
We hope that you have found this information useful. If you have any questions or are worried about anything, please speak to the Dorset County Hospital dtaff on the above numbers.
About this leaflet
Authors: Dr Shobhana Marathe, Mr Usama Faridi
Written: October 2025
Approved: January 2026
Review date: January 2029
Edition: 1.1
If you have feedback regarding the accuracy of the information contained in this leaflet, or if you would like a list of references used to develop this leaflet, please email patientinformation.leaflets@dchft.nhs.uk
Print leaflet