Angle-closure Glaucoma and Laser Iridotomy
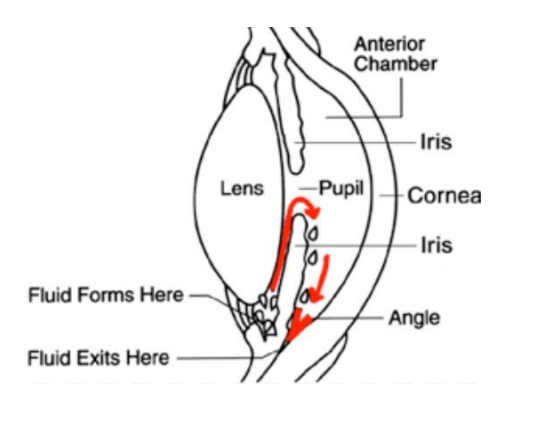
The eye is filled with a clear fluid, called aqueous, which circulates within the front chambers of the eye. The aqueous fluid is produced behind the iris and it flows forward through the pupil and drains through the drainage angle. The drainage angle area is in the gap between the edge of the iris and cornea (see diagram below).
There are two main groups of glaucoma, angle-closure and open-angle types, depending on whether the drainage pathway is blocked, or not, respectively. Although open-angle glaucoma is more common, the angle-closure glaucoma is a more severe disease, with a greater risk of blindness.
Some people, usually people who are longsighted, tend to develop narrow drainage angles. Throughout life, the human lens grows and takes up more space within the eye. This can make the drainage angle even narrower as one gets older. Eventually, this can lead to a complete blockage of the angle (angle-closure) and raised eye pressure. This may occur suddenly, causing severe pain, nausea, vomiting, and blurred vision. If not treated promptly, permanent sight loss can occur. This is a condition known as acute angle-closure glaucoma.
Sometimes blockage to the drainage occurs gradually, over many years. Patients may have a high pressure within the eye that they are unaware of which can potentially lead to damage to the optic nerve and loss of vision. This condition is known as chronic angle-closure glaucoma.
Treatment options for narrow drainage angles
- Laser iridotomy is the preferred line of treatment as it is the least invasive procedure to open the drainage channels in your eye.
- Sometimes having a cataract operation can widen the drainage channels and help ease the pressure inside your eye.
- Age-related growth of the lens plays a major part in the mechanisms leading to primary angle-closure glaucoma; therefore, lens extraction (cataract surgery) is used routinely in patients who also have cataract.
- In patients without cataract, clear-lens extraction could be a reasonable option to consider in some cases, such as in patients with severe refractive errors, where the quality of vision is not improved with their glasses. According to a major clinical study, it is a reasonable option to consider in people over 50 years of age. The consultant will discuss this with you.
- The regular use of Pilocarpine eye drops helps to open the drainage channels; however, these are not always an effective choice of treatment. The drops can cause side effects such as blurred vision, headaches and possible cataract formation.
Laser iridotomy
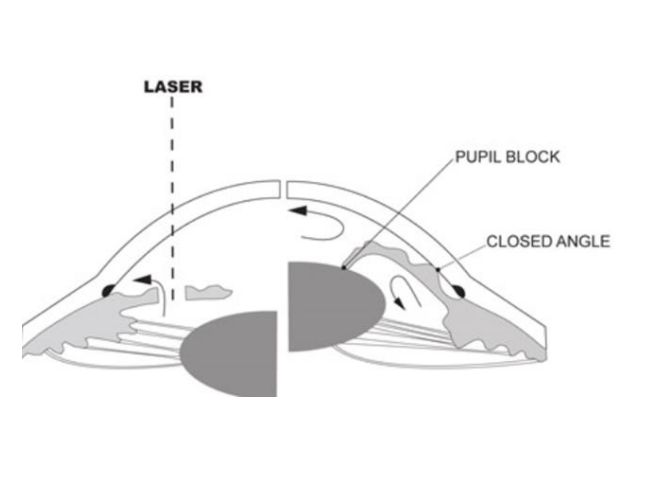
Laser iridotomy involves creating a small hole within the iris (coloured part of the eye) using laser therapy. This is usually at the very edge of the iris and usually at the top portion of the eye.
The iridotomy enables an alternative path for the passage of aqueous from the posterior chamber to the anterior chamber of the eye. It is the commonest procedure for treating angle-closure glaucoma. As our eyes are usually very symmetrical in structure, the other eye will also be at risk, therefore, both eyes are likely to be treated.
How do I know if I am at risk of angle closure?
Your optician or ophthalmologist will be able to identify whether you are at risk by examining the drainage angle in the front of your eye. New imaging techniques, such as Optical Coherence Tomography (OCT) scans, are commonly used these days to assess the drainage angle width and identify suspected cases.
In some cases, people may develop symptoms, such as seeing coloured halos around lights, eye pain, and headaches. If this happens, contact your optician or GP straight away.
What does laser iridotomy involve?
The procedure is performed in the outpatients department and usually takes a few minutes.
You will be given eye drops before the procedure to make the pupil small and prevent a raise in eye pressure, which may occur after treatment. The drops can sometimes cause headaches which may last for one to two hours. You will be asked to sit in the waiting area until the drops have had time to work.
The specialist performing the laser will put anaesthetic drops in your eye to numb the surface.
During the treatment, you will be sat upright with your chin resting on a machine similar to the one you are examined on in the eye clinic.
A contact lens is placed on the surface of your eye which helps focus the laser beam and stops you from blinking. This lens requires a small amount of lubricating eye gel to help protect your eye and improves the specialist’s view.
The laser procedure is not usually painful, but you may experience a slight stinging sensation within the eye. Sometimes the laser causes a tiny amount of bleeding within the eye. If this happens the specialist will press firmly with the contact lens on the eye for a minute or so, which usually stops it. Your vision can be slightly blurred after the procedure, but will generally clear after a few hours.
The doctor may ask you to return 30-60 minutes after your treatment for a check of your intraocular pressure by the staff nurse. Occasionally there can be a slight rise in pressure following the procedure and you may require a brief period of treatment with pressure-lowering drops and possible surgical intervention if necessary.
After the procedure you will be given a prescription for a five to seven day course of steroid drops to minimise any inflammation. Do not drive yourself to the appointment but arrange for someone else to bring you.
How will I know the procedure has worked?
An appointment will be made for you a few weeks after the procedure for your eye to be re-examined. If the procedure has been successful, the drainage site will appear to have ‘opened up’ and this reduces the risk of developing glaucoma.
However, there remains a risk of developing chronic glaucoma in the future and you should continue to have face to face reviews with your optician if discharged from the eye clinic.
If the drainage angle remains narrow after the iridotomy, you may benefit from a different type of laser called laser iridoplasty. Your check-up should identify if this applies to you and the specialist will explain this in more detail.
What are the benefits of laser iridotomy?
- It reduces the risk of a sudden (acute) severe rise in eye pressure
- It makes you less likely either to develop angle-closure or for the condition to get worse
- It reduces the future risk of an acute attack of glaucoma that can happen with the dilation procedures of the pupil
- It reduces the risk of blindness from glaucoma
- Please note that it will not make your eyesight better, or give you back the sight you have already lost from glaucoma
- A major clinical study showed laser 5410 iridotomy treated eyes had about 50% reduction in risk of progression to primary angle closure compared with untreated eyes.
Are there any risks of the procedure?
The laser iridotomy is considered safe but, as with any procedure, there is a small element of risk which includes:
- Brief blurred vision lasting for a few hours
- Failure or closure of the iris hole created by laser and occasionally the procedure needs to be repeated (1% of cases)
- Minor bleeding in the eye is common (about 30% of cases). Patients taking warfarin should have had a blood test within the last week confirming an INR within the therapeutic levels. Please tell us if you are taking any blood-thinning medicines and bring your yellow book with you if you are on Warfarin
- Intraocular pressure may rise following the procedure but is usually temporary (1% of cases)
- Occasionally the pressure spike is persistent, which could include drops, tablets, injection, or occasionally surgery (0.1% risk)
- Worsening of the clouding lens (cataract) and laser injury to the lens capsule
- Rarely, double vision, ghosting of vision or glare sensations may occur, due to the awareness of light entering through the new hole in the iris (10% of cases)
- Corneal burns occur in less than 1% of cases
- Retinal haemorrhage and detachment (very rare)
- The risk of vision loss or the need for urgent surgery following the procedure is extremely rare (around one in 5,000).
Contact numbers
We hope that you have found this information useful. If you have any questions or are worried about anything, please speak to the following Dorset County Hospital staff:
Department: 01305 255410 / 01305 255980
Secretary: 01305 255846
About this leaflet
Authors: Mr Usama Faridi, REI Consultant and RGN Christine Lush
Written: July 2020
Updated and approved: February 2022
Review date: February 2025
Edition: v2
If you have feedback regarding the accuracy of the information contained in this leaflet, or if you would like a list of references used to develop this leaflet, please email patientinformation.leaflets@dchft.nhs.uk
Print leaflet